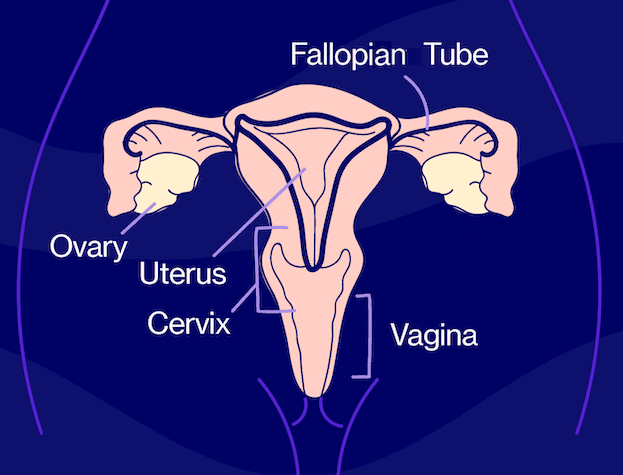
Decreased libido is defined as a low desire, drive, or motivation for any type of sexual activity, as well as the lack of sexual fantasies or thoughts.
Narrowing it down to a singular cause is difficult since there can be several intersecting mental and physical factors that contribute, including:

Fluctuating hormones & physical changes:
As hormone levels shift and ultimately decline during the menopausal transition, so too can interest in sex. Interesting fact: Testosterone, the main hormone of desire, is an androgen that typically peaks in your 20s and steadily declines throughout the menopause transition, playing a major role in low libido.
Another result of hormone changes? Vaginal dryness. Because here is the thing: without sufficient estrogen/oestrogen and testosterone supply, vaginal tissues aren’t as moist as they once were, which leads to…you guessed it…dryness (and decreased elasticty). A technical – and somewhat outdated – term for this is atrophy of vaginal tissues (a more updated and comprehensive term is “genitourinary syndrome of menopause” or, the more pronounceable acronym, GSM). Upwards of 30% of women experience it in perimenopause, and 75% postmenopause. With dryness comes painful or uncomfortable sex as well as weakened sexual arousal and orgasm — and let’s be real: that’s not the kind of sex anyone would want to have (or should be having), which at least partly explains the low libido.
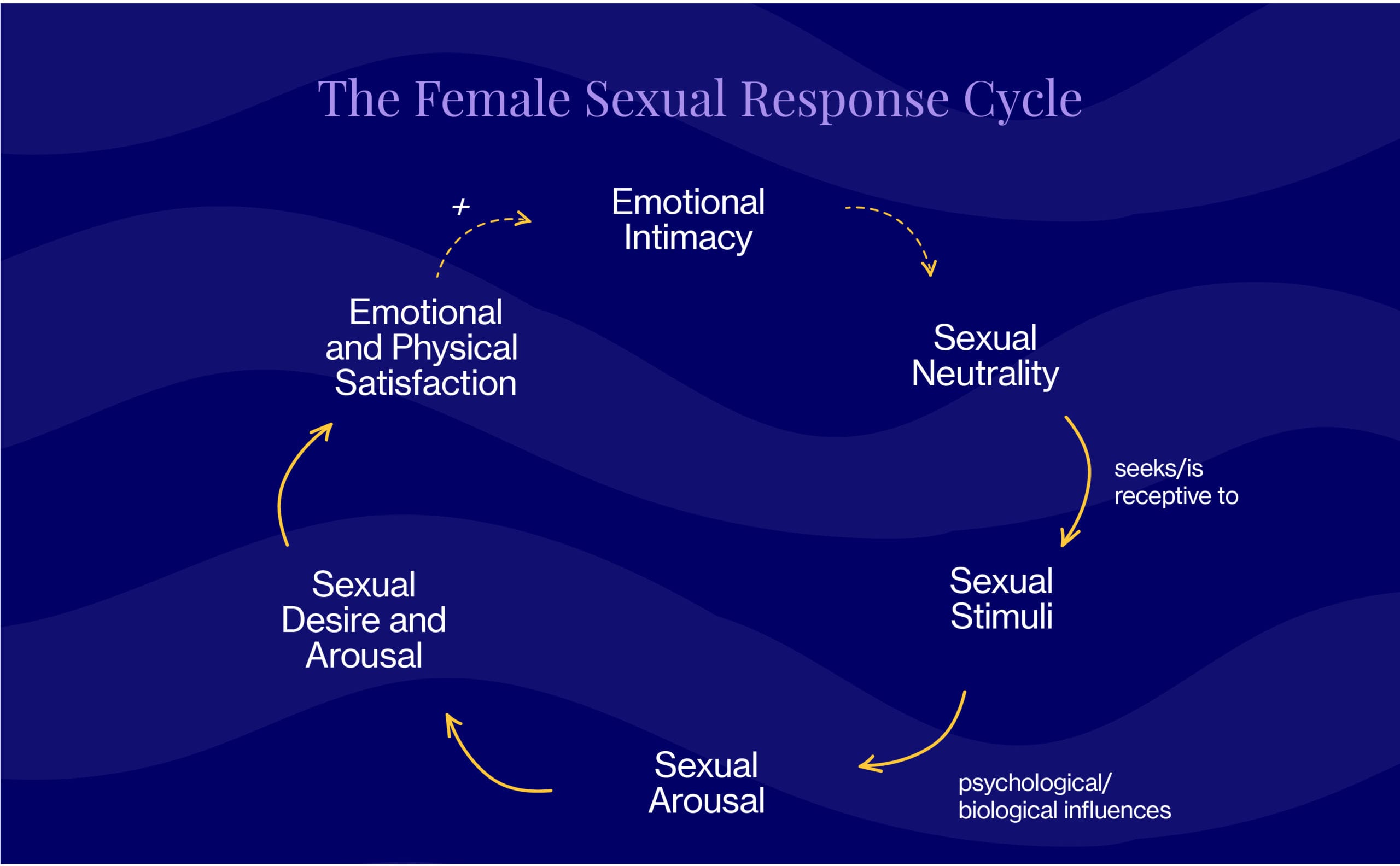
Leave it to Dr. Rosemary Basson, Director of the University of British Columbia’s Sexual Medicine Program, to prove to the world that there’s no one single reason people choose to have sex. Departing from traditional thinking, Dr. Basson created the circular, more complex model shown below, which acknowledges that a whole slew of relationship factors affect one’s willingness and ability to participate in sex. It also acknowledges that desire can be either responsive or spontaneous, and come before or after arousal. And while orgasm may contribute to satisfaction, it is not (we repeat, not) necessary for it. Oh, and you can totally enter the cycle at different points, too.
Emotional & behavioral factors:
Fatigue, stress, mood swings, relationship hurdles, and struggles with body image are things many, if not all, women experience during their lifetime. Nothing revolutionary there. But many of us don’t realize just how important of a role these emotional and behavioral factors play when it comes to intimacy, which is closeness and connectedness with a partner, either physical, emotional, or both. Intimacy is often the trigger needed for sexual desire and arousal in women.
Without emotional intimacy, the chances of sexual desire are slim. And without sexual desire, there’s no sexual activity. And repeat, and repeat.
Also worth noting is the fact that certain medications, specifically antidepressants and those used to treat heart disease and diabetes, have side effects that can contribute to a decrease or loss of libido. Even some over-the-counter medications such as antihistamines (are you taking Claritin all spring?) can cause dryness and, in turn, low desire.
In some cases, low libido that persists for at least six months, negatively affects your life, and is not due to another co-existing medical/psychiatric condition or medication is diagnosed as Hypoactive Sexual Desire Disorder (HSDD). While prevalence rates vary, research suggests that HSDD affects 10% of adult females — meaning you’re 100% not alone.
Your healthcare provider may recommend FDA-approved medications, herbal supplements, and/or behavioral modifications to manage HSDD symptoms (more on that below).
READ MORE:
- Low Libido: The Unspoken Menopause Symptom (let’s fix that)
- Setting The Record Straight On Orgasms During & After Menopause
- Sex Should *Never* Hurt. So How Come It Sometimes Does During Menopause?
Dr. Anna Barbieri, MD
Pro tip #1
A few things to keep in mind when it comes to sexual health...sex does not require a partner and does not exclusively mean intercourse. Intimacy with yourself is *just* as important as partnered sex — and it’s good for your overall well-being! Masturbation relieves built-up stress, helps you sleep better, boosts your mood, helps you relax, relieves cramps...we could go on and on. We’ve highlighted some of the best tools out there to help you achieve all of these benefits.