Published on Mar 08, 2022
Last modified on Apr 17, 2023
A Hysterectomy Expert on What to Know about Surgical Menopause

We recently caught up with one of our favorite medical experts, Philip M. Sarrel, M.D., Professor Emeritus of OB/GYN and Psychiatry at Yale on what women need to know about surgical menopause due to hysterectomy. As the Founder and President of the Advancing Health After Hysterectomy (AHAH) foundation, which is devoted to educating women and healthcare professionals on this topic, there’s truly no one better to ask. Below we’ve highlighted the key takeaways we should all know about one of the biggest taboos in an already-stigmatized space.
What is one piece of advice that every woman facing surgical menopause should know?
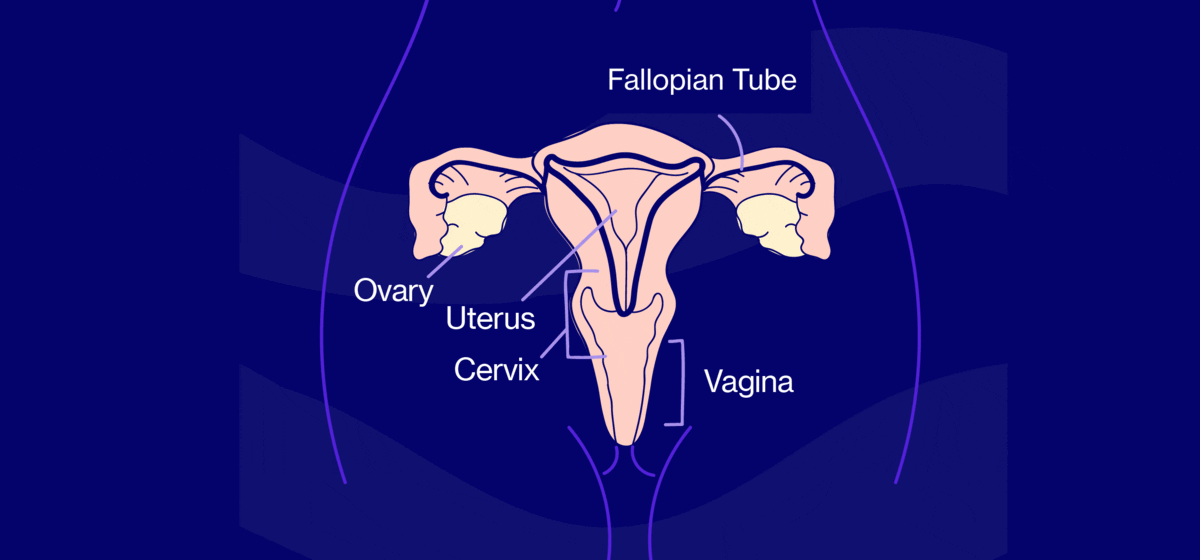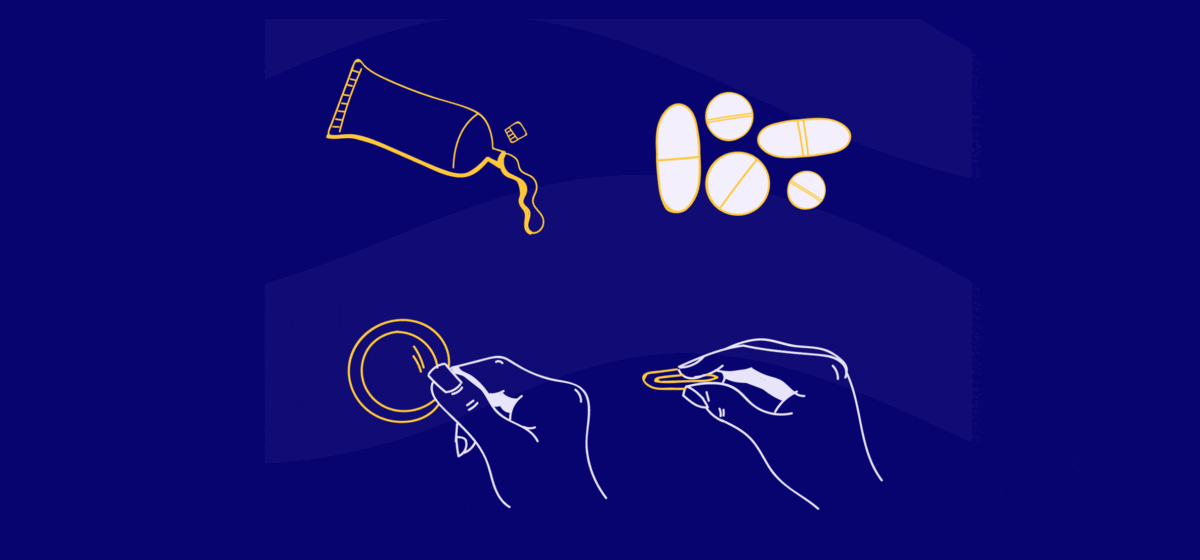
She should know that her ovarian hormone production will be affected by a hysterectomy – the procedure in which the uterus is surgically removed – whether her ovaries are removed or not. (Check out the diagram for a quick refresher of the anatomy in question.) As a result, she may experience hormone withdrawal symptoms immediately, even while still in the hospital. It’s appropriate for her to ask if her surgeon is prepared to prescribe estradiol (also known as estrogen) replacement therapy either before or soon after the surgery.

Hysterectomy accounts for half of the women under age 50 who are menopausal.
What is one common misconception about surgical menopause?
A common misconception is that conserved ovaries – those that remain even after the uterus is removed – will continue to function normally.
The most common age range for hysterectomies and oophorectomies are between 40-44 and the second most common range is between 35-39. For the women under age 45 especially, the surgeon will typically try to conserve the ovaries, but half of these women will have their ovaries removed at the time of surgery anyway.
During the procedures, almost all ovaries have a period of ischemia (an inadequate blood supply to an organ) and infarction (an obstruction of the blood supply to an organ, causing local death of the tissue). Within 6 months following the procedure, an estimated 1/4 women are hypoestrogenic (estrogen deficient). After 3 years, that percentage grows to 40%. This means that it is important to monitor hormone levels in the months and years following surgery, diagnose, and treat estrogen deficiency if and when it occurs. The women whose ovaries are removed are immediately hypoestrogenic and should have estradiol replacement prescribed. They may also need testosterone replacement (but not necessarily immediately).
It is estimated more than 100,000 women have died in the last 20 years because of estrogen avoidance.
Why are you personally passionate about hysterectomy awareness?
Hysterectomy accounts for half of the women under age 50 who are menopausal. In the 1940s it was clearly documented that the loss of estrogen at a young age predisposes women to developing osteoporosis and cardiovascular disease. Recent studies indicate that estrogen replacement (meaning, estrogen therapy) after hysterectomy lowers the risk for developing sexual dysfunction and depression, dementia, stroke, breast and colon cancer, and all-cause mortality (translation: any cause for death) before age 70. Health insurance costs and patient healthcare visits are markedly reduced in women who use estrogen after hysterectomy.
These findings are recorded in the long-term Women’s Health Initiative (WHI) reports and studies such as the Mayo Clinic Oophorectomy study. Prior to the WHI report in 2002, more than 90% of women used estrogen replacement after surgery to effectively treat menopause symptoms and reduce disease and mortality risks. The WHI study scared healthcare professionals and women themselves. As a result, current use of estrogen for any significant time is less than 10% after hysterectomy.
The result? Recent generations of women are experiencing an “alarming rate” of hospitalizations for acute myocardial infarction (commonly known as a heart attack). It is estimated more than 100,000 women have died in the last 20 years because of estrogen avoidance.
The current data has led the American Heart Association to publish a Scientific Position Statement advocating the use of estrogen therapy in women age 45 and younger who have undergone surgical menopause. For more information, connect with an Elektra Health clinician here.
Philip M. Sarrel, M.D., has been a member of Yale University School of Medicine’s OB/GYN and Psychiatry faculty since the 1960s. In 1975, he started Yale’s Menopause Program. His late wife, Lorna Sarrel, was a pioneering figure in the fields of human sexuality, psychiatry, and the psycho-social aspect of menopause. Together, they directed the Yale Sex Counseling Service for 40 years. Dr. Sarrel has written six books and published over 200 articles in medical journals. In 2014, he founded the Advancing Health After Hysterectomy Foundation.

Dr. Phil and Lorna Sarrel pictured with Jannine Versi, Elektra co-founder, December 2019.
READ MORE:
Navigating Life After Surgical Menopause: What to Know & How to Prepare



